Table of Contents
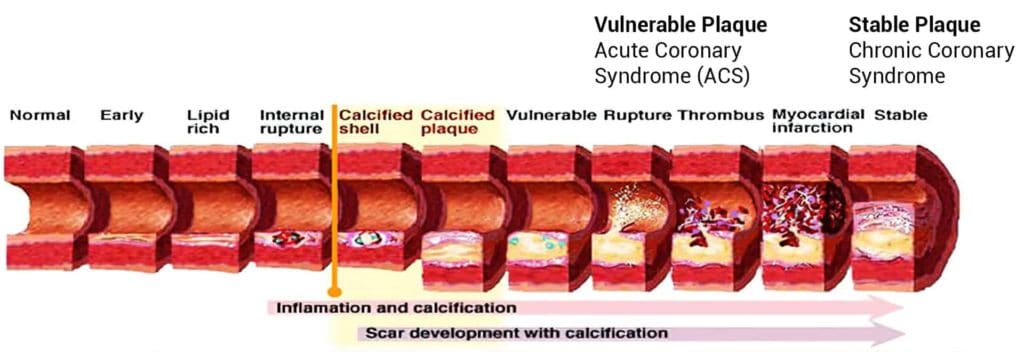
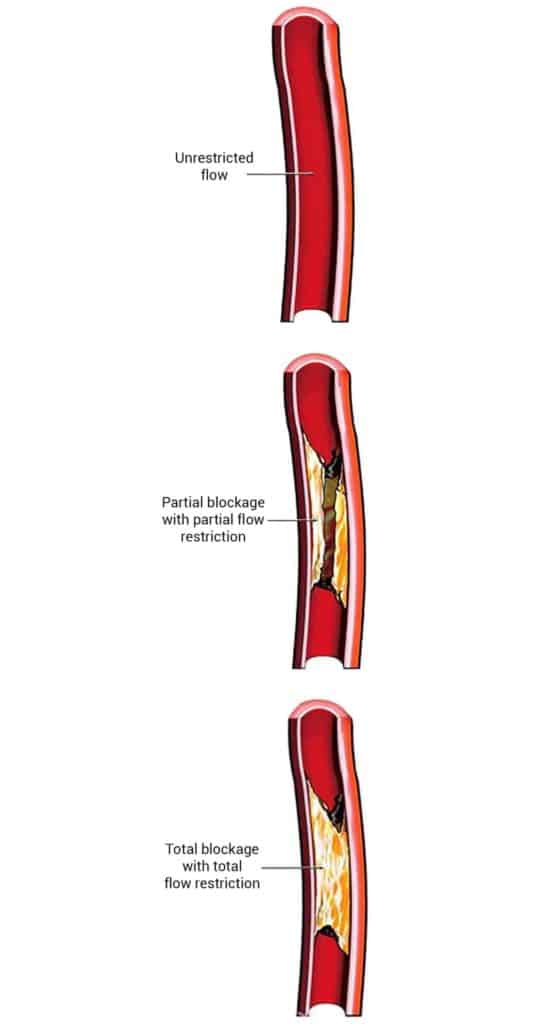
ToggleHeart blockage, also known as coronary artery disease, occurs when the coronary arteries become narrowed or blocked, reducing blood flow to the heart muscle. This is most commonly caused by the gradual buildup of plaque, made up of cholesterol, fatty deposits, and other substances, along the artery walls. Over time, this narrowing can limit oxygen supply to the heart, especially during physical activity or stress. If a plaque ruptures, it can trigger a sudden blockage and lead to a heart attack.
According to the Centers for Disease Control and Prevention, coronary artery disease remains one of the most common types of heart disease, reinforcing the importance of early detection and prevention.
What Causes Heart Blockage and How It Develops
The most common cause of heart blockage is coronary atherosclerosis, a condition where plaque builds up along the walls of the coronary arteries. Over time, this buildup narrows the arteries and reduces blood flow to the heart muscle.
If left untreated, plaque can continue to accumulate, leading to stable coronary artery disease, where symptoms may occur during physical activity. If a plaque ruptures, it can trigger the formation of a blood clot that suddenly blocks the artery, resulting in acute coronary syndrome (ACS), which includes heart attacks.
Less common causes of heart blockage include:
- Coronary artery spasm: A temporary tightening of the artery that reduces blood flow
- Coronary artery vasculitis: Inflammation of the coronary arteries
Coronary Atherosclerosis (Blocked Arteries)
Coronary atherosclerosis is the most common cause of heart blockage and is often used interchangeably with coronary artery disease. It occurs when plaque, made up of cholesterol, fatty deposits, calcium, and other substances, gradually builds up along the walls of the coronary arteries.
As plaque accumulates over time, it narrows the arteries and reduces blood flow to the heart. This can lead to stable coronary artery disease, where symptoms such as chest discomfort may occur during physical activity or stress.
If a plaque becomes unstable and ruptures, it can trigger the rapid formation of a blood clot. This may suddenly block the artery, resulting in acute coronary syndrome (ACS), which includes heart attacks and requires immediate medical attention.
Coronary artery spasm
Coronary artery spasm is a less common cause of heart blockage. It occurs when the muscles within the artery wall suddenly tighten, temporarily narrowing the artery and reducing blood flow to the heart muscle.
Unlike typical angina, which is often triggered by physical activity, coronary artery spasms tend to occur at rest, most commonly between midnight and early morning. This condition is also known as Prinzmetal’s angina, vasospastic angina, or variant angina.
Common triggers include:
- Tobacco use
- Exposure to cold temperatures
- Severe emotional stress
Use of stimulant drugs, such as amphetamines or cocaine
Coronary artery vasculitis (CAV)
Coronary artery vasculitis (CAV) is a rare cause of heart blockage involving inflammation of the coronary arteries. This may occur as an isolated condition or as part of a broader systemic inflammatory disease affecting multiple organs.
Several underlying conditions are associated with CAV, including Kawasaki disease, Takayasu’s arteritis, polyarteritis nodosa, and giant cell arteritis. Unlike atherosclerosis, which typically affects older adults, CAV is more commonly seen in younger individuals.
Inflammation of the coronary arteries can lead to a range of complications, including artery narrowing (stenosis), aneurysm formation, and blood clot (thrombus) development. These changes can impair blood flow and may result in acute coronary events if not appropriately managed.
What Are the Risk Factors for Heart Blockages?
As coronary atherosclerosis is the most common cause of heart blockage, the key risk factors are those that contribute to plaque buildup in the arteries. These can be broadly divided into modifiable and non-modifiable factors.
Modifiable risk factors:
- High cholesterol: Elevated LDL cholesterol contributes to plaque formation in the arteries
- High blood pressure (hypertension): Damages artery walls and accelerates narrowing
- Diabetes: Increases inflammation and affects blood vessel health
- Smoking: Promotes plaque buildup and reduces oxygen supply to the heart
- Unhealthy diet: Diets high in saturated fats, salt, and processed foods increase cardiovascular risk
- Physical inactivity: Reduces cardiovascular efficiency and contributes to weight gain
- Obesity or excess weight: Associated with multiple risk factors such as hypertension and diabetes
- Chronic stress: May indirectly increase risk through its effects on blood pressure and lifestyle habits
Non-modifiable risk factors:
- Age: Risk increases as arteries naturally stiffen over time
- Family history of heart disease: Genetic predisposition can increase susceptibility
Many of these risk factors can be managed through lifestyle changes and appropriate medical care, significantly reducing the risk of developing coronary artery disease.
What Are the Consequences of Heart Blockages?
Heart blockage can lead to a range of complications depending on how the condition develops. These may occur gradually over time or suddenly, depending on plaque stability and overall cardiovascular risk.
Chronic progression: Stable coronary artery disease
When heart blockage develops gradually and remains untreated, it can lead to progressive myocardial ischaemia, where the heart muscle receives insufficient oxygen.
This often results in worsening symptoms over time, including chest discomfort and reduced exercise tolerance. This stage is commonly referred to as stable coronary artery disease or chronic coronary syndrome, where symptoms are typically triggered by physical activity or stress.
Acute progression: Acute coronary syndrome
In some cases, plaque within the artery may rupture suddenly, often triggered by physical or emotional stress. This can lead to the rapid formation of a blood clot, causing a partial or complete blockage of the artery.
This condition is known as acute coronary syndrome (ACS) and includes heart attacks. It is a medical emergency and carries a significantly increased risk of severe complications or death if not treated promptly.
What Are the Symptoms of Heart Blockages or Blocked Arteries?

Heart blockage may not always present with clear or early symptoms. In some cases, the first sign can be a serious event such as a heart attack or even sudden cardiac death. Studies suggest that a significant proportion of sudden cardiac deaths are linked to underlying coronary artery disease, sometimes without prior warning signs.
However, many patients do experience symptoms as the condition progresses, particularly when blood flow to the heart becomes more restricted.
Common symptoms include:
- Chest discomfort (angina): Pressure, tightness, or heaviness in the chest
- Shortness of breath: Especially during physical activity
- Fatigue: Reduced energy or decreased exercise tolerance
- Pain radiating to the upper body: Arms, neck, jaw, or shoulders
- Dizziness or lightheadedness
It is important to note that some individuals, especially those with diabetes, may experience mild or no symptoms, a condition often referred to as “silent” coronary artery disease.
What Is the Treatment for Heart Blockages/Blocked Arteries?
Treatment for heart blockage focuses on addressing the underlying cause, improving blood flow to the heart, and reducing the risk of future complications. Management is typically approached in a stepwise manner, often described as a therapeutic pyramid, where treatment intensity increases based on severity.
Lifestyle changes (Foundation of Treatment)
The base of the therapeutic pyramid involves adopting a healthier lifestyle. This includes:
- Stopping smoking
- Following a heart-healthy diet
- Increasing regular physical activity
- Managing stress and maintaining a healthy weight
Long-term success depends on consistency and adherence to these changes, as they play a key role in slowing disease progression.
Medications (Targeted Medical Management)
If lifestyle changes alone are insufficient, medications may be prescribed to manage risk factors and symptoms. The choice of medication depends on the underlying cause and individual risk profile.
Common types include:
- Antiplatelet agents (e.g. aspirin, clopidogrel): Help reduce the risk of blood clot formation
- Anti-anginal medications (e.g. calcium channel blockers): Improve blood flow by relaxing coronary arteries
- Beta-blockers: Reduce the workload on the heart
- Statins: Lower cholesterol levels and help stabilise plaque
In specific conditions such as coronary artery vasculitis, immune-modulating medications may also be required.
Revascularisation procedures (PCI and CABG)
In more advanced cases where medications are not sufficient, procedures may be required to restore adequate blood flow to the heart.
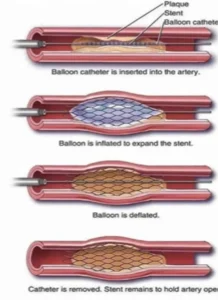
- Percutaneous coronary intervention (PCI): A minimally invasive procedure in which a catheter is used to open a narrowed artery, usually followed by the placement of a stent to keep it open.
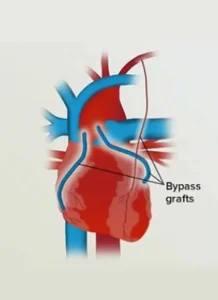
- Coronary artery bypass grafting (CABG): A surgical procedure that creates a new pathway for blood flow by bypassing the blocked artery using a vessel from another part of the body.
- Hybrid approach: In selected cases, a combination of PCI and CABG may be used to achieve the best outcome.
The choice of procedure depends on factors such as the number and location of blockages, the number of vessels involved, heart function, and any co-existing medical conditions. Treatment decisions are individualised and made in consultation with a cardiologist.

What Are the Procedures for Heart Blockage/Blocked Arteries?
Procedures for heart blockage focus on both accurate diagnosis and, when necessary, restoring blood flow to the heart. The choice of procedure depends on the severity and location of the blockage, as well as your overall condition.
Assessment of the coronary arteries
Invasive coronary angiography (ICA)
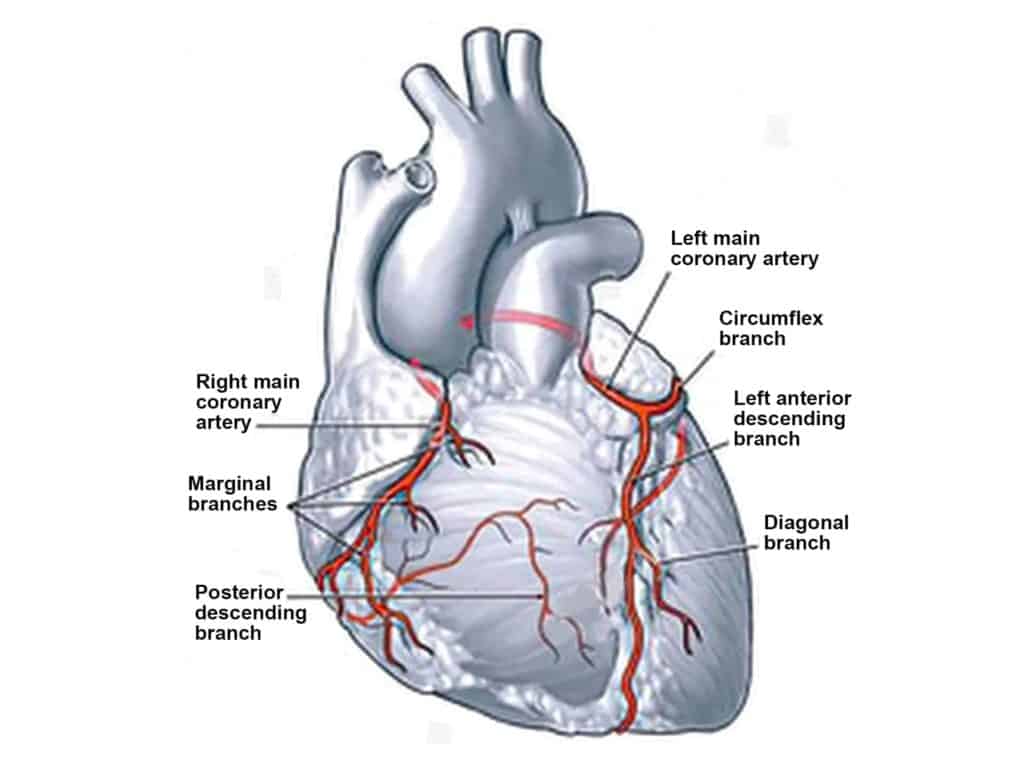
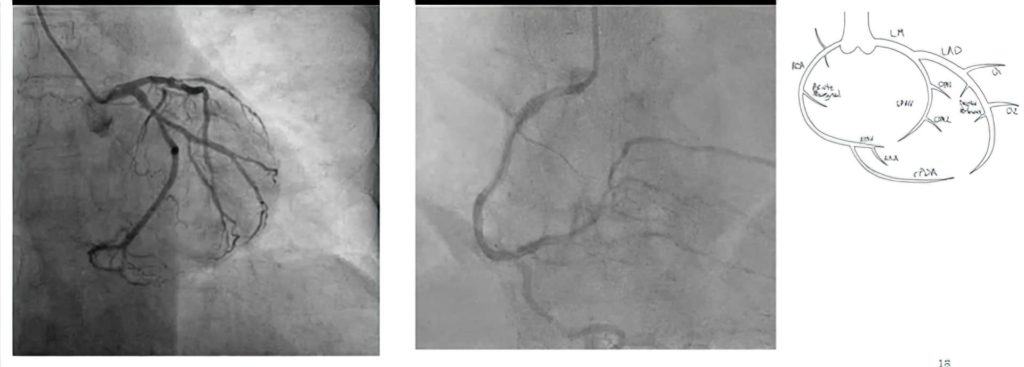
Invasive coronary angiography is considered the gold standard for evaluating coronary artery blockages. It provides detailed images of the arteries and helps determine the severity and exact location of any narrowing.
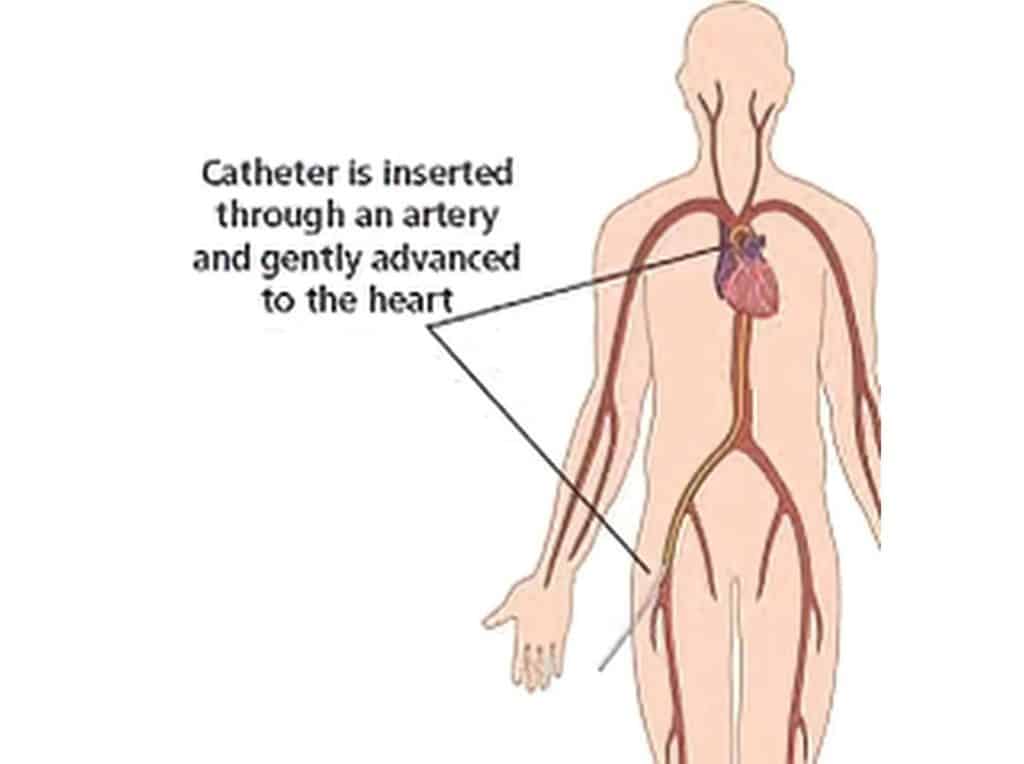
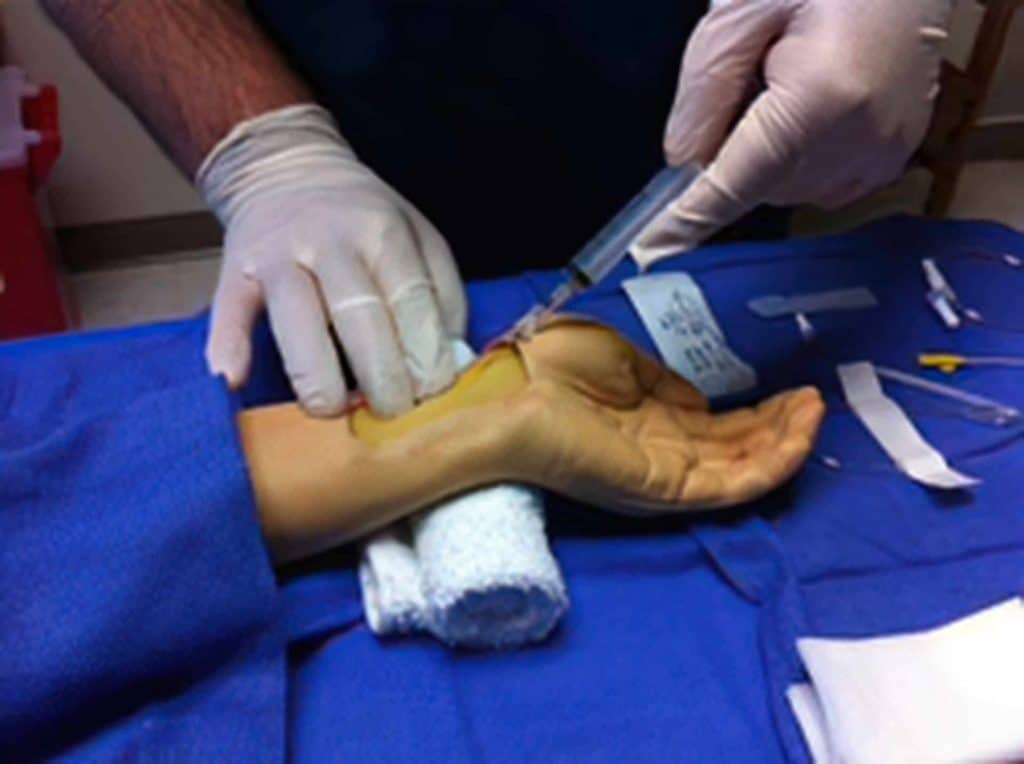
During the procedure, a thin and flexible catheter is inserted through an artery, usually in the wrist (radial artery) or groin (femoral artery), and guided towards the heart. A contrast dye is then injected, and X-ray imaging is used to visualise the coronary arteries in real time.
This allows the cardiologist to accurately assess blood flow and decide whether further treatment, such as angioplasty or surgery, is required.
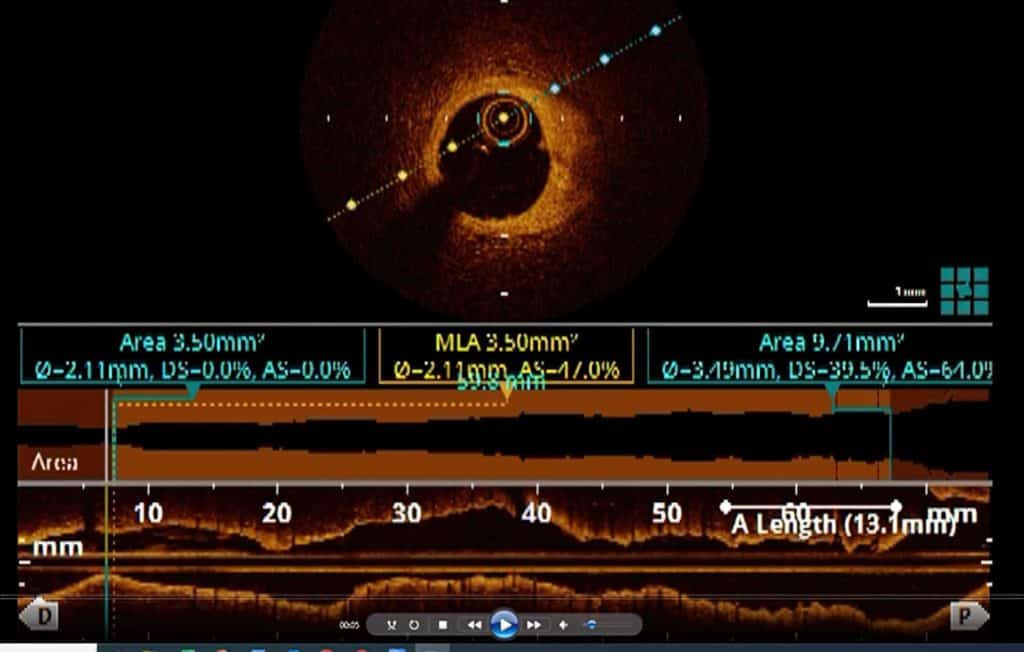
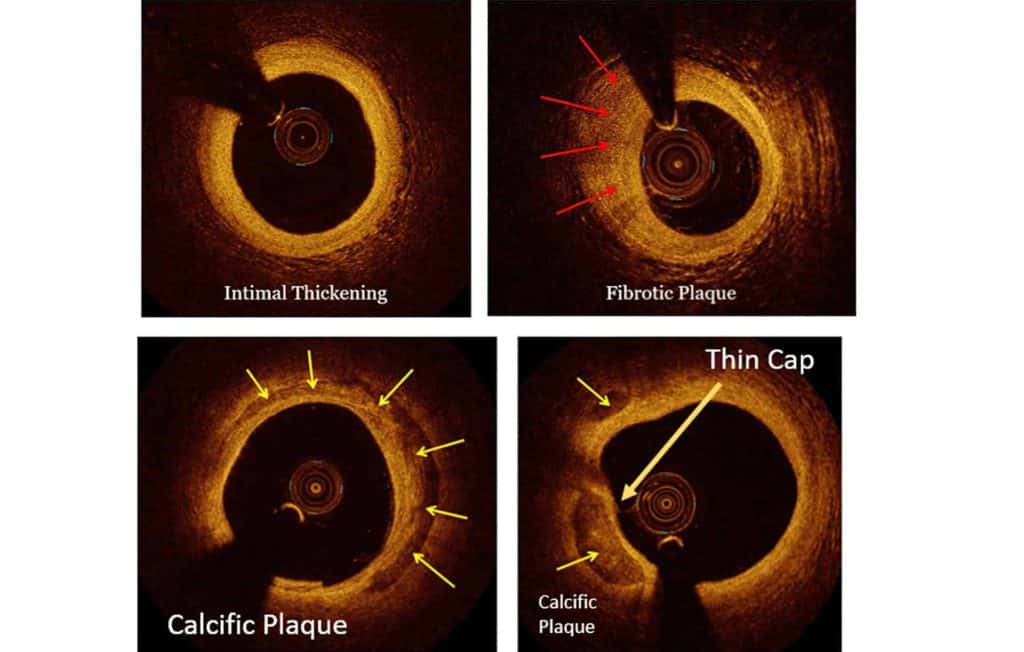
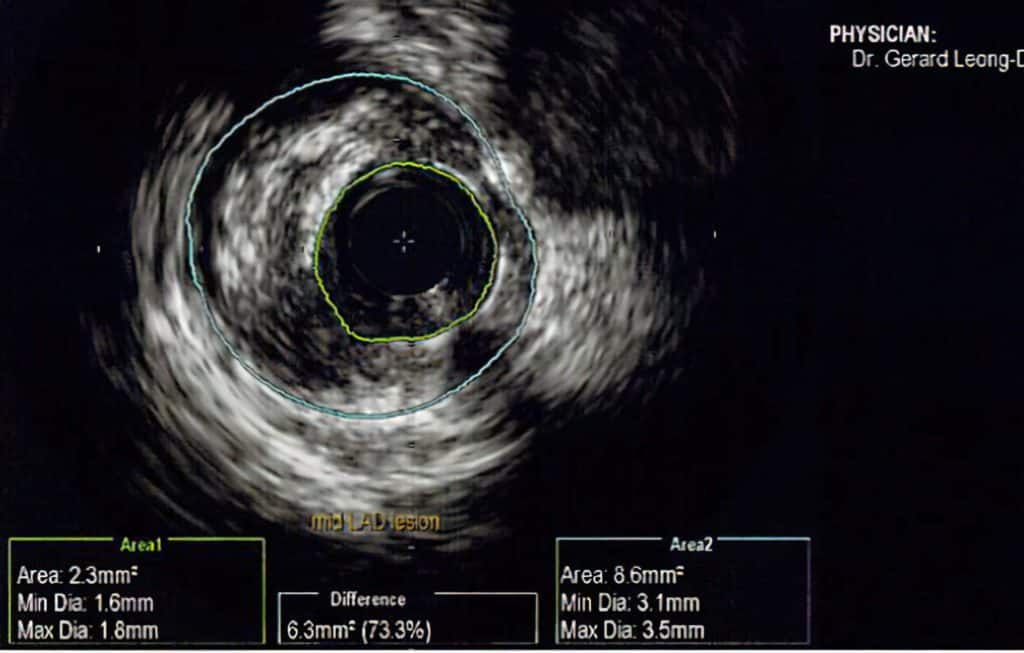
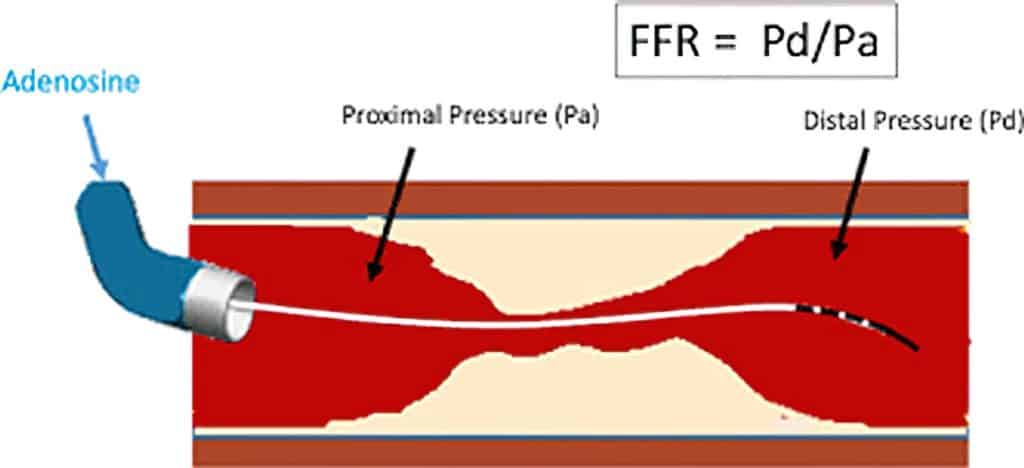
Supplementary Modalities for Coronary Artery Assessment
In addition to coronary angiography, several specialised techniques may be used to provide more detailed information about the arteries. These are typically performed during the same procedure to further assess the severity and characteristics of the blockage.
Take Control of Your Heart Health
Heart blockage is a serious but manageable condition when identified early and treated appropriately. Understanding how it develops, recognising symptoms, and knowing your treatment options can make a meaningful difference in long-term outcomes.
If you have risk factors such as high blood pressure, high cholesterol, diabetes, or a family history of heart disease, it is important to take a proactive approach. Early assessment allows for timely intervention and helps reduce the risk of complications.
At Gerard Leong Cardiology Clinic, we provide comprehensive evaluation and personalised care for patients at every stage of heart health, from preventive screening to advanced treatment. Our focus is on accurate diagnosis, evidence-based management, and long-term cardiovascular care.
Frequently Asked Questions
Can heart blockage develop even if I feel completely healthy?
Yes. Heart blockage can develop silently over time without noticeable symptoms. Some individuals only discover it during routine screening or after a cardiac event, which is why regular check-ups are important, especially if you have risk factors.
Is heart blockage the same as high cholesterol?
No. High cholesterol is a risk factor, not the condition itself. Heart blockage occurs when plaque builds up in the arteries, often as a result of long-term elevated cholesterol levels and other contributing factors.
Can younger individuals develop heart blockage?
Although more common in older adults, heart blockage can occur in younger individuals, particularly those with risk factors such as smoking, obesity, diabetes, or genetic predisposition.
How long does it take for heart blockage to develop?
Heart blockage typically develops gradually over many years due to ongoing plaque accumulation. However, complications such as a heart attack can occur suddenly if a plaque ruptures.
Can lifestyle changes alone be enough to manage heart blockage?
In early or mild cases, lifestyle changes may be sufficient to slow progression and improve heart health. In more advanced cases, medications or procedures may be required alongside lifestyle modifications.